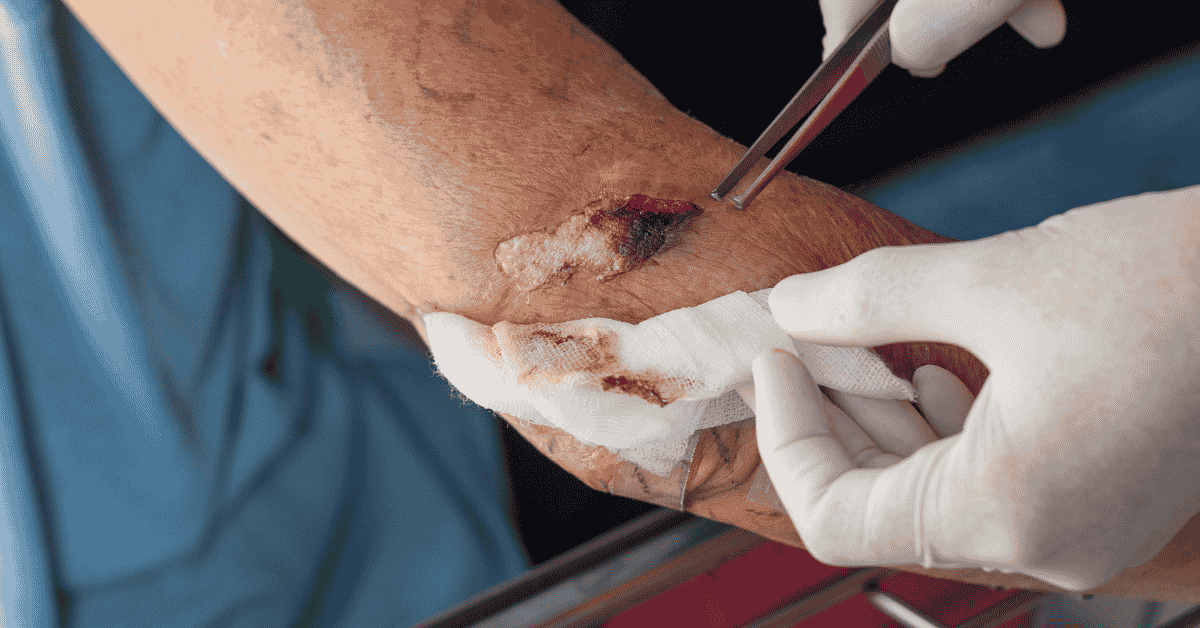
Sever wound surgery is a highly specialized branch of trauma medicine designed to manage deep, complex, and often life-threatening injuries that involve extensive damage to skin, muscle, nerves, blood vessels, or bone. This type of surgical intervention is performed when a wound is too severe to heal through natural recovery or basic medical treatment. In most cases, sever wound surgery is required immediately after traumatic events such as accidents or violent injuries to prevent complications like infection, tissue death, or permanent functional loss. The procedures involved are often multi-layered, combining emergency stabilization with reconstructive techniques. Medical teams must evaluate the injury carefully to determine the extent of damage before selecting the appropriate surgical approach. Because of its complexity, sever wound surgery is typically performed in trauma centers equipped with advanced surgical technology. The goal is not only to close the wound but also to restore function and prevent long-term disability.
Causes and Risk Factors Behind Severe Wounds
Severe wounds that require sever wound surgery often result from high-energy trauma that overwhelms the body’s natural protective barriers. Motor vehicle accidents remain one of the most common causes, especially those involving high-speed impact or crushing forces. Workplace injuries in construction, manufacturing, and heavy machinery environments also frequently lead to deep lacerations and tissue destruction. Falls from significant heights can cause both external wounds and internal structural damage that require surgical correction. Sports injuries, particularly in contact sports, may result in torn ligaments, deep cuts, or compound fractures. Burns caused by fire, electricity, or chemicals can destroy multiple layers of tissue, making reconstructive surgery necessary. In some cases, untreated infections or chronic diseases such as diabetes significantly worsen wound severity, turning minor injuries into surgical emergencies.
Clinical Assessment and Diagnostic Evaluation
Before performing sever wound surgery, a detailed clinical assessment is essential to determine the severity and complexity of the injury. Medical professionals first stabilize the patient by addressing life-threatening conditions such as bleeding or shock. Vital signs are continuously monitored to ensure the patient can safely undergo surgical intervention. Imaging techniques such as X-rays, CT scans, and MRI scans are used to evaluate bone fractures, soft tissue damage, and internal injuries. Blood tests help detect infection markers, blood loss levels, and clotting abnormalities. The wound is carefully examined for contamination, foreign objects, and tissue viability. These diagnostic steps allow surgeons to develop a precise and safe surgical plan tailored to the patient’s condition.
When Sever Wound Surgery Becomes Necessary
Sever wound surgery is required when tissue damage exceeds the body’s natural healing capacity. One major indication is the presence of necrotic tissue that must be surgically removed to prevent infection spread. Deep wounds exposing muscles, tendons, or bones also require immediate surgical repair to restore structural integrity. Uncontrolled bleeding that cannot be managed through external pressure is another critical indication. Sever wound surgery is also necessary when blood flow to the injured area is compromised, risking tissue death. Open fractures where bone is exposed or shattered require surgical stabilization and reconstruction. Severe infections that penetrate deep into tissue layers also demand surgical intervention to prevent systemic complications.
Surgical Procedures Used in Sever Wound Surgery
Several surgical techniques are used depending on the nature and severity of the wound. Surgical debridement is often the first step, involving the removal of dead or infected tissue to create a clean environment for healing. Wound closure techniques such as suturing or stapling are used when tissue edges can be safely brought together. Skin grafting is frequently performed when large areas of skin are lost, using healthy skin from another part of the body. Flap surgery involves transferring tissue with its own blood supply to reconstruct complex wounds. Microvascular surgery allows surgeons to repair small blood vessels and restore circulation in damaged areas. Orthopedic surgical methods may be required when fractures or bone damage are present alongside soft tissue injuries.
Preoperative Preparation and Surgical Planning
Careful preparation is essential before performing sever wound surgery to ensure patient safety and successful outcomes. The patient is first stabilized to address any immediate life-threatening conditions such as shock or severe bleeding. Anesthesia is selected based on the severity of the wound and may range from local to general anesthesia. The surgical site is thoroughly cleaned and sterilized to reduce infection risk. Antibiotics are often administered before surgery to prevent bacterial contamination. Imaging results are reviewed to guide the surgical approach and avoid unexpected complications. The surgical team coordinates each step to ensure precision and efficiency during the procedure.
Step-by-Step Surgical Process
The surgical process begins with a thorough exploration of the wound to assess internal damage. Damaged or dead tissue is carefully removed through debridement to promote healthy healing. Bleeding is controlled using surgical tools such as cauterization or vessel ligation techniques. Surgeons then repair damaged structures including muscles, tendons, and blood vessels. If necessary, reconstructive procedures such as grafts or flaps are applied to restore tissue coverage. The wound is then closed using appropriate methods depending on tension and tissue condition. Drainage systems may be placed to prevent fluid accumulation and reduce infection risk. Finally, sterile dressings are applied to protect the surgical site.
Postoperative Care and Monitoring
After sever wound surgery, careful postoperative care is essential for proper healing. Wound dressings are regularly changed under sterile conditions to prevent infection. Pain management is provided through prescribed medications tailored to the patient’s condition. Antibiotic therapy continues to reduce the risk of bacterial infection. Patients are closely monitored for signs of complications such as swelling, redness, or discharge. Follow-up appointments allow doctors to assess healing progress and make necessary adjustments. In some cases, early physical movement is encouraged to improve circulation and prevent stiffness.
Healing Stages After Sever Wound Surgery
Healing after sever wound surgery occurs in multiple biological stages that support tissue repair. The first stage involves blood clot formation, which helps stop bleeding and protect the wound. The inflammatory stage follows, where the immune system removes bacteria and damaged cells. During the proliferative stage, new tissue begins to form and gradually fills the wound area. The remodeling stage strengthens the repaired tissue and improves flexibility over time. Healing speed depends on factors such as age, nutrition, and overall health condition. Proper medical care throughout each stage is essential for optimal recovery.
Complications and Post-Surgical Risks
Although sever wound surgery is highly effective, complications may still occur during recovery. Infections are one of the most common risks, especially in deep or contaminated wounds. Delayed healing may occur due to poor circulation or underlying medical conditions. Nerve damage can lead to loss of sensation or reduced mobility in the affected area. Excessive scar formation may restrict movement or affect appearance. Blood clots can develop in severe trauma cases and require immediate attention. Graft rejection is another possible complication in reconstructive procedures.
Rehabilitation and Functional Restoration
Rehabilitation plays a crucial role in restoring function after sever wound surgery. Physical therapy helps rebuild strength, flexibility, and mobility in affected areas. Occupational therapy assists patients in returning to daily activities such as walking, dressing, or working. Customized exercise programs are designed based on the severity of injury and surgical outcomes. Scar management techniques help improve skin elasticity and appearance over time. Psychological support may also be necessary for patients recovering from traumatic injuries. Long-term rehabilitation ensures full recovery and improved quality of life.
Special Medical Considerations
Certain patient groups require additional care during sever wound surgery and recovery. Patients with diabetes often experience slower healing due to reduced blood circulation. Elderly individuals may have fragile skin and weaker regenerative abilities, requiring specialized treatment plans. Pediatric patients need carefully designed surgical approaches to support growth and development. Individuals with vascular diseases face increased risks due to poor blood flow. Each case requires personalized medical strategies to ensure safe and effective recovery outcomes.
Innovations in Sever Wound Surgery
Modern advancements have significantly improved outcomes in sever wound surgery. Negative pressure wound therapy enhances healing by improving blood flow and removing excess fluid. Bioengineered skin substitutes provide alternatives for patients with extensive skin loss. Advanced imaging systems allow surgeons to plan procedures with high precision. Minimally invasive surgical tools reduce trauma and shorten recovery time. Microsurgical techniques enable detailed repair of small blood vessels and nerves. These innovations continue to improve survival rates and functional recovery.
Emergency Indicators Requiring Immediate Care
Certain symptoms indicate the need for immediate medical attention before or after sever wound surgery. Deep wounds exposing bone, muscle, or tendons require urgent evaluation. Uncontrolled bleeding that does not stop with pressure is a medical emergency. Signs of infection such as fever, redness, or pus formation require immediate treatment. Loss of movement or sensation may indicate nerve damage or structural injury. Severe swelling and discoloration can signal internal complications. Early intervention significantly improves treatment outcomes.
Preventive Strategies for Severe Injuries
Preventing injuries that lead to sever wound surgery involves adopting safety measures in daily life. Wearing protective gear in high-risk environments reduces the likelihood of severe trauma. Following road safety regulations helps prevent traffic-related injuries. Proper handling of tools and machinery minimizes workplace accidents. Managing chronic conditions like diabetes reduces complications from minor wounds. Prompt treatment of small injuries prevents them from developing into severe surgical cases.
Frequently Asked Questions (FAQ)
What is sever wound surgery used for?
Sever wound surgery is used to treat deep injuries involving skin, muscles, bones, or blood vessels that cannot heal naturally.
How long does recovery take after sever wound surgery?
Recovery varies depending on injury severity and may take weeks to several months.
Is sever wound surgery painful?
The procedure itself is not painful due to anesthesia, but recovery may involve some discomfort.
What are the risks of sever wound surgery?
Risks include infection, scarring, delayed healing, nerve damage, and graft complications.
Can severe wounds heal without surgery?
Most severe wounds require surgical intervention to heal properly and avoid complications.
Is rehabilitation necessary after surgery?
Yes, rehabilitation is essential for restoring movement, strength, and function.
Takeaway
Sever wound surgery remains a vital medical intervention for treating complex traumatic injuries that cannot heal through conventional methods. Its success depends on timely diagnosis, precise surgical techniques, and structured postoperative care. With advancements in medical technology and rehabilitation strategies, patients now have improved chances of full recovery and restored functionality.