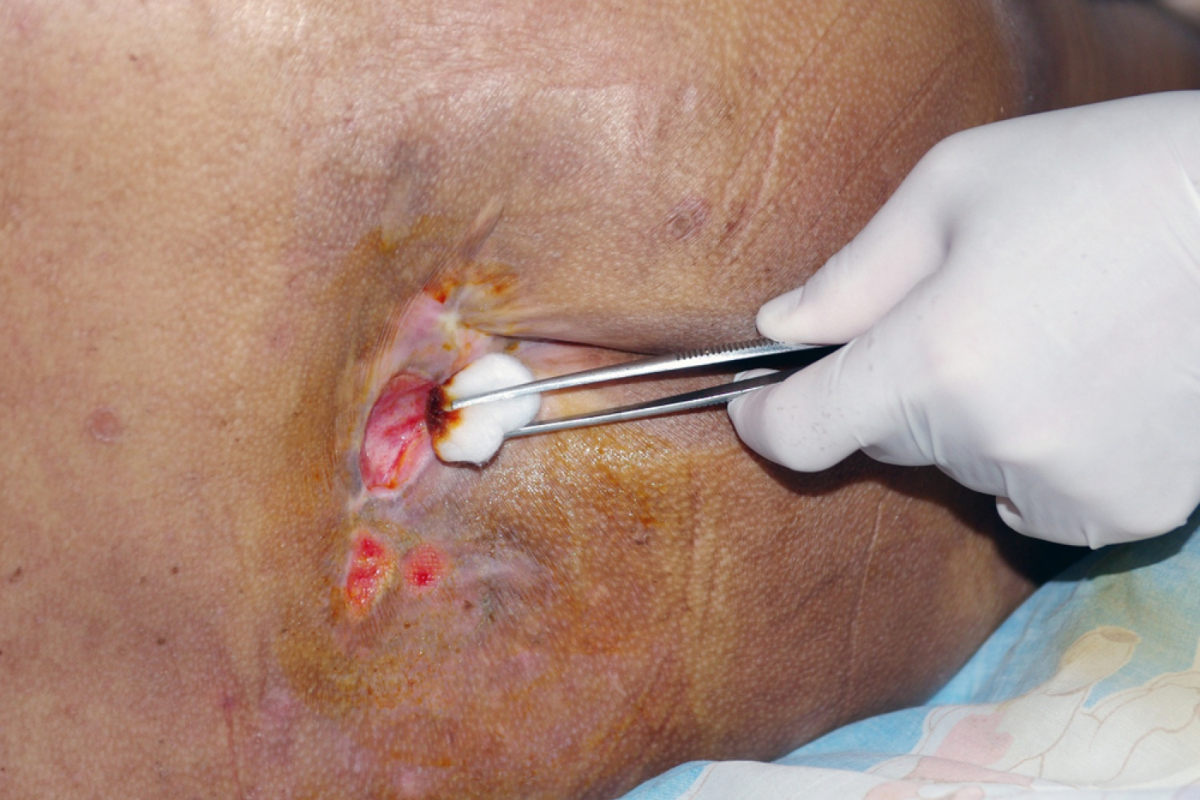
What Decubitus Ulcers Are and Why They Develop
Decubitus ulcers, often referred to as pressure sores or bedsores, are localized injuries that occur when sustained pressure disrupts blood flow to the skin and underlying tissues. These wounds typically form over bony areas such as the tailbone, hips, heels, and shoulders. When circulation is restricted for extended periods, the affected tissue begins to break down, leading to visible damage. Individuals with limited mobility are particularly susceptible, including those confined to beds or wheelchairs. Early signs may include redness, warmth, or tenderness in specific areas of the skin. If left unaddressed, these mild symptoms can quickly progress into deeper and more serious wounds. Recognizing how these ulcers develop is essential for implementing effective decubitus ulcer treatment strategies.
Key Risk Factors That Increase Vulnerability
A variety of conditions and circumstances can heighten the risk of developing pressure ulcers. Immobility remains the most significant factor, as it prevents regular pressure relief on certain parts of the body. Friction caused by movement against bedding or clothing can weaken the skin’s protective barrier. Shear forces, which occur when the skin moves in one direction while the underlying tissue moves in another, can also cause damage. Moisture from perspiration or incontinence contributes to skin breakdown by softening and weakening the tissue. Poor nutrition and dehydration further reduce the body’s ability to repair damaged skin. Chronic illnesses such as diabetes or circulatory disorders make healing more difficult. Understanding these risks is essential for both prevention and effective decubitus ulcer treatment.
Recognizing the Different Stages of Pressure Ulcers
Pressure ulcers are classified into stages to determine the extent of tissue damage and guide appropriate care. Stage 1 is characterized by intact skin with noticeable redness or discoloration that does not fade when pressed. Stage 2 involves partial skin loss, often presenting as a blister or shallow open sore. Stage 3 indicates deeper tissue damage where fat may be visible, signaling a more serious condition. Stage 4 is the most severe, involving extensive damage that can reach muscles, tendons, or bone. Some ulcers are labeled unstageable when covered by dead tissue, making it difficult to assess their depth. Deep tissue injuries may appear as dark patches beneath intact skin, indicating hidden damage. Accurate staging is critical for selecting the most effective decubitus ulcer treatment approach.
Essential Components of Decubitus Ulcer Treatment
Treating pressure ulcers effectively requires a combination of consistent care and medical intervention. Relieving pressure on the affected area is the first and most important step in preventing further damage. Repositioning the patient at regular intervals helps restore proper blood flow and supports healing. Keeping the wound clean reduces the risk of infection and promotes tissue repair. Proper dressing techniques protect the wound while maintaining an optimal healing environment. Pain management is also an important aspect, as discomfort can limit mobility and slow recovery. Supporting overall health through balanced nutrition enhances the body’s ability to heal. These combined efforts form the backbone of successful decubitus ulcer treatment.
Effective Wound Care Methods
Wound care plays a central role in managing and healing pressure ulcers. Cleaning the wound with appropriate solutions removes bacteria and debris that may interfere with recovery. Debridement is often necessary to remove dead tissue and stimulate new growth. There are several methods available, including surgical, enzymatic, and autolytic approaches. Selecting the right dressing helps maintain moisture balance and protects the wound from contamination. Regular monitoring ensures that any changes in the wound are addressed promptly. Caregivers must also pay attention to the surrounding skin to prevent additional breakdown. Consistency in wound care practices is essential for achieving positive results in decubitus ulcer treatment.
Key Steps in Daily Wound Management
- Gently cleanse the wound using recommended solutions
- Apply dressings suited to the ulcer’s stage and condition
- Remove dead tissue through safe and appropriate methods
- Check for signs of infection such as swelling or unusual discharge
- Keep surrounding skin dry and protected
- Follow a consistent schedule for dressing changes
- Record observations to track healing progress
Advanced Therapies for Severe Cases
When standard treatments are not enough, advanced medical therapies may be required. Negative pressure wound therapy uses controlled suction to promote tissue growth and remove excess fluids. Biologic dressings and growth factors can help accelerate the healing process by encouraging cell regeneration. Hyperbaric oxygen therapy increases oxygen supply to the wound, which may improve recovery in certain cases. Surgical interventions such as skin grafts or flap reconstruction are sometimes necessary for deep or non-healing ulcers. These procedures are typically performed under the supervision of specialized healthcare professionals. Advanced treatments are often recommended for patients with complex or long-standing wounds. Access to these options can significantly improve outcomes in challenging decubitus ulcer treatment situations.
Enhancing Comfort Through Pain Management
Pain associated with pressure ulcers can range from mild discomfort to severe distress, depending on the stage of the wound. Managing this pain is crucial for improving the patient’s overall experience and encouraging mobility. Medications such as pain relievers or anti-inflammatory drugs are commonly used to control symptoms. Non-medical approaches, including repositioning and supportive surfaces, can also provide relief. Gentle handling during dressing changes minimizes additional discomfort. Emotional support is equally important, as chronic wounds can affect mental health. Creating a calm and supportive environment helps patients cope more effectively. Addressing pain is an integral part of comprehensive decubitus ulcer treatment.
The Impact of Nutrition on Healing
Proper nutrition is a key factor in the body’s ability to repair damaged tissue. Protein plays a vital role in rebuilding skin and supporting immune function. Vitamins such as Vitamin C contribute to collagen production, which is essential for wound healing. Minerals like zinc and iron support tissue repair and oxygen transport. Adequate hydration helps maintain skin elasticity and overall health. Patients who struggle to meet their nutritional needs may benefit from supplements. A well-balanced diet tailored to individual needs can significantly enhance recovery. Integrating nutrition into decubitus ulcer treatment ensures a more effective healing process.
Preventing Future Pressure Ulcers
Preventing the recurrence of pressure ulcers requires ongoing care and vigilance. Regular repositioning helps reduce prolonged pressure on vulnerable areas of the body. Supportive devices such as specialized mattresses and cushions improve weight distribution and comfort. Routine skin inspections allow for early detection of potential issues. Maintaining cleanliness and managing moisture levels protect the skin from breakdown. Educating caregivers and patients on proper techniques promotes consistency in care. Small daily actions can make a significant difference in preventing new ulcers. These preventive measures are essential for long-term success in decubitus ulcer treatment.
Choosing Between Home Care and Medical Support
The decision to manage pressure ulcers at home or seek professional care depends on the severity of the condition. Mild ulcers can often be treated at home with proper guidance and attention to detail. Caregivers play a crucial role in ensuring consistent wound care and monitoring progress. However, more advanced ulcers require medical expertise to prevent complications. Warning signs such as increased pain, infection, or delayed healing should not be ignored. Regular consultations with healthcare providers help ensure that the treatment plan remains effective. Combining home care with professional support often yields the best results. Making informed decisions about care is essential for successful decubitus ulcer treatment.
Challenges That May Affect Recovery
Managing pressure ulcers can be a complex process with several potential obstacles. Chronic health conditions can slow healing and increase the risk of complications. Infections remain a major concern, particularly in deeper wounds. Limited mobility can make it difficult to relieve pressure consistently. Adhering to treatment plans requires commitment from both patients and caregivers. Financial constraints may limit access to advanced therapies or specialized equipment. Emotional stress can also impact the overall healing process. Addressing these challenges requires a comprehensive and adaptable approach to decubitus ulcer treatment.
Frequently Asked Questions
What is the most important step in decubitus ulcer treatment
Relieving pressure on the affected area is the most critical step, as it prevents further tissue damage and allows healing to begin.
Can pressure ulcers heal without medical treatment
Mild cases may improve with proper care, but more severe ulcers require medical attention to avoid serious complications.
How can caregivers help prevent pressure ulcers
Caregivers can assist by repositioning patients regularly, maintaining hygiene, and monitoring skin condition closely.
What complications can arise from untreated pressure ulcers
Untreated ulcers can lead to infections, tissue death, and even life-threatening conditions if not managed properly.
Are there specific foods that help with healing
Foods rich in protein, vitamins, and minerals support tissue repair and strengthen the immune system.
When should a doctor be consulted
Medical advice should be sought if the ulcer worsens, shows signs of infection, or does not improve with basic care.
Takeaway
Decubitus ulcer treatment involves a combination of attentive care, medical support, and preventive strategies to ensure effective healing. Addressing pressure, maintaining proper wound care, and supporting the body through nutrition all contribute to better outcomes. Patients and caregivers must remain consistent in their efforts to manage and monitor the condition. Advanced treatments provide additional options for more severe cases, offering improved chances of recovery. Preventive measures play a vital role in avoiding recurrence and maintaining skin health. With the right approach, managing pressure ulcers becomes more achievable and less overwhelming.