Bed sores, also known as pressure ulcers, are a common concern for individuals dealing with chronic conditions such as diabetes, paralysis, or limited mobility. Proper bed sore treatment is essential for preventing serious complications and ensuring long-term health. Chronic patients are especially vulnerable due to reduced circulation, weakened skin, and slower healing processes, making early intervention and expert care crucial. Kalingap Wound Care Clinic provides specialized solutions designed to address these unique challenges, offering comprehensive management for bed sores.
Understanding Bed Sores in Chronic Conditions
Chronic conditions can significantly increase the risk of bed sores. Conditions such as diabetes, cardiovascular diseases, and long-term immobility affect blood flow, skin resilience, and tissue recovery. Individuals confined to beds or wheelchairs for extended periods are particularly susceptible. Bed sore treatment for chronic patients requires a careful understanding of these underlying factors, along with targeted interventions to protect vulnerable areas like the heels, hips, tailbone, and elbows. Recognizing the impact of chronic illnesses on skin health allows caregivers and healthcare providers to plan effective prevention and treatment strategies.
Signs and Stages of Bed Sores
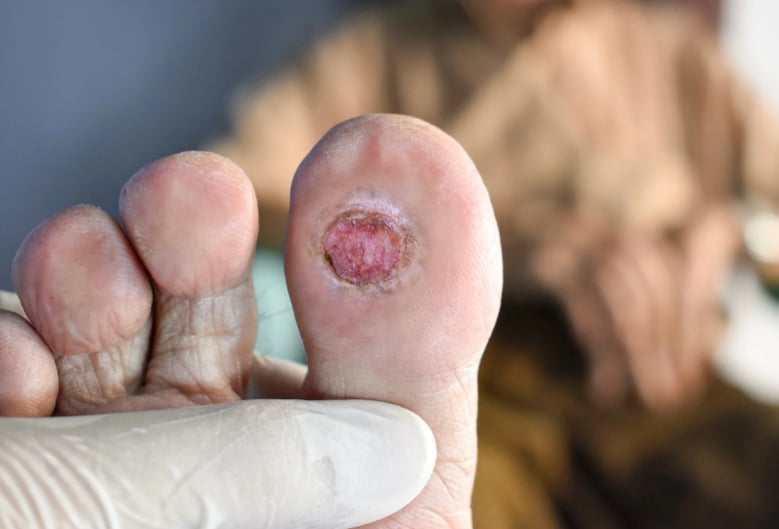
Recognizing bed sores early is critical for effective bed sore treatment. Pressure ulcers are categorized into four stages:
- Stage 1: Reddened skin that does not blanch when pressed. Early intervention can prevent progression.
- Stage 2: Partial-thickness skin loss, often appearing as an open sore or blister.
- Stage 3: Full-thickness skin loss involving damage to subcutaneous tissue.
- Stage 4: Extensive tissue damage, potentially affecting muscle, tendons, or bone.
Monitoring these stages enables caregivers to implement bed sore treatment promptly, reducing the risk of infection and long-term complications.
Causes of Bed Sores in Chronic Conditions
Bed sores develop due to prolonged pressure on the skin, friction, moisture, poor nutrition, and limited mobility. Chronic illnesses often exacerbate these risk factors. For instance, diabetes can reduce circulation, slowing tissue repair, while immobility increases pressure on specific areas of the body. Effective bed sore treatment requires addressing both the immediate wound and the contributing factors to prevent recurrence. Understanding these causes allows caregivers and medical professionals to develop tailored strategies for each patient.
Prevention Strategies for Bed Sores
Preventing bed sores is a critical part of overall bed sore treatment. Frequent repositioning and the use of pressure-relieving devices, such as specialized mattresses and cushions, can dramatically reduce risk. Maintaining skin hygiene and keeping the skin dry and clean prevents irritation and infection. Proper nutrition supports tissue repair and overall skin health, making it a vital component of bed sore treatment. Caregivers should monitor high-risk patients daily for early signs of pressure ulcers to ensure timely intervention.
Treatment Options for Bed Sores
Treatment of bed sores for chronic conditions ranges from at-home care to professional medical intervention. At-home care includes gentle cleaning, dressing changes, pressure relief, and monitoring for signs of infection. Professional bed sore treatment, however, is often necessary for advanced wounds. Kalingap Wound Care Clinic offers specialized services, including expert assessment, advanced dressings, infection management, and personalized care plans. Engaging professional care ensures that chronic patients receive timely and effective treatment, significantly improving outcomes.
Advanced Bed Sore Treatments for Chronic Conditions
Advanced therapies can accelerate healing and prevent complications in chronic patients. Techniques such as negative pressure wound therapy, hydrocolloid and foam dressings, and regenerative therapies are increasingly effective for severe or non-healing sores. In some cases, surgical intervention may be required. Kalingap Wound Care Clinic provides access to these modern bed sore treatment options, offering tailored solutions that meet the specific needs of chronic patients. Utilizing advanced therapies under expert supervision improves recovery speed and reduces the risk of recurrence.
Choosing the Right Care Provider
Selecting the right care provider is essential for successful bed sore treatment in chronic conditions. Clinics specializing in wound care provide personalized treatment plans, consistent monitoring, and professional expertise. Kalingap Wound Care Clinic stands out as a trusted partner, offering compassionate care and evidence-based approaches. Patients benefit from expert guidance, comprehensive management, and continuous support, ensuring a higher quality of life and faster healing.
Patient and Caregiver Tips
Daily monitoring and early intervention are essential components of bed sore treatment. Caregivers should assist patients in repositioning, ensure proper nutrition, and maintain clean and dry skin. Educating both patients and caregivers about risk factors, warning signs, and appropriate interventions enhances recovery outcomes. Emotional support and patience are equally important, as chronic patients may require long-term care and attention. Kalingap Wound Care Clinic provides guidance and training to caregivers, ensuring that patients receive the most effective care possible.
Takeaway
Effective bed sore treatment for chronic conditions requires early detection, preventive strategies, and professional care. Chronic patients face unique challenges that demand personalized attention and advanced therapies. Kalingap Wound Care Clinic delivers expert solutions, compassionate care, and specialized wound management, making it the ideal partner for individuals at risk of pressure ulcers. Timely intervention and expert guidance can significantly improve healing, reduce complications, and enhance the overall quality of life for chronic patients.
Frequently Asked Questions (FAQ)
1. What is the fastest way to heal a bed sore in chronic patients?
Prompt professional intervention, regular wound care, proper nutrition, and pressure relief are essential for fast healing.
2. How often should chronic patients be repositioned to prevent bed sores?
Patients should be repositioned at least every two hours to reduce pressure on vulnerable areas.
3. Can bed sores in chronic conditions be fully healed?
Yes, with consistent care, advanced treatment, and professional supervision, bed sores can heal completely.
4. What are the signs that a bed sore needs professional treatment?
Signs include deep tissue damage, persistent pain, redness, pus, or non-healing sores despite home care.
5. How does Kalingap Wound Care Clinic personalize bed sore treatment?
The clinic evaluates each patient’s condition, develops a tailored care plan, provides advanced therapies, and monitors progress for optimal recovery.